Millions of people replace their missing teeth with dental implants each year. There is no question that dental implants offer the best solution to replacing your missing teeth. However, preparing for implant surgery can be somewhat nerve-wracking, especially if this is your first implant. Just like with any other surgery, it's normal to experience some level of pain and discomfort following your surgery. The good news is that implant surgeries usually hurt less than tooth extractions. This is because dental implants mostly deal with the jawbone and gum tissue, which aren't as sensitive as teeth. In other words, if you've managed to pull your tooth, you should be able to handle the implant surgery as well.
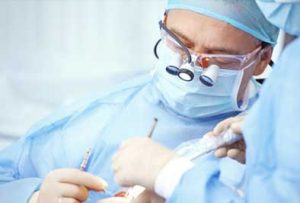
Dental implant surgery generally hurt less than tooth extraction
What should you do before implant surgery?
Preparing for dental implant surgery is somewhat similar to preparing for any other surgery. Be sure to follow your dentist's instructions carefully. Here are some general guidelines to help ease the process and speed up your recovery:
Take Your Medications

It's quite common that your dentist prescribes you medications to help with the surgery and recovery process. Dentists usually prescribe antibiotics and painkillers for most implant surgeries. Additionally, you might be given a special mouthwash to use before surgery. Taking prophylactic medications can be helpful. It expedites the healing process, decreases post-op pain, and reduces the likelihood of developing infections. Be sure to take your medications as instructed by your dentist.
If you take your own prescribed medications continue taking them as you normally would, unless advised otherwise by your dentist. For example, if you're taking pills for high blood pressure, diabetes, a thyroid condition, etc. then you should continue taking your medications up until and after the implant surgery. There are a few medications that interfere with implant surgery. The most important ones are blood thinner medications. Blood thinners such as Warfarin and Plavix require extra precaution. The newer generation blood thinners, such as Pradaxa, Xarelto, and Eliquis are safer to take during implant surgery. Regardless, you need to consult with your physician as to whether or not you should discontinue your blood thinner. Your physician, not the dentist, will decide whether or not you should continue or discontinue your blood thinner before implant surgery.
There are also a few medical issues that you need to be mindful of prior to your implant surgery. For example, if you've had a recent stent or artificial joint, such as a hip or knee replacement, then you must pre-medicate before implant surgery. Pre-medication protects the artificial limbs against the sudden spike of bacteria in the bloodstream and reduces the likelihood of a serious infection. The current recommendation is that you should pre-medicate if you've had a stent or artificial joint replacement within the past two years. The pre-medication protocol involves taking a high dose of Amoxicillin (2,000 mg) or Clindamycin (600 mg) an hour before implant surgery. Consult with your physician to see if you need to pre-medicate in advance.
Diet Before Implant Surgery
It's best to eat something before any oral surgery. First off, having something in your stomach helps regulate your sugar levels. Secondly, eating reduces saliva flow which maintains a drier working area for your dentist. Finally, there's a pretty good chance that you won't be able to eat a solid meal for a good while after the surgery. So eat a hearty meal and show up on time for your appointment. This also applies to patients undergoing IV sedation. For sedation, it's best to eat a light meal and avoid drinking too many liquids. Also, no coffee or any other stimulants beforehand. If you're scheduled to undergo general anesthesia then you must fast overnight since eating before surgery is no longer permitted.
Relax!

The last thing you should do before surgery is stressing out. Stress increases your blood pressure which makes it harder to administer local anesthetics. Yep, you need more shots to get numb if you're too stressed! Stress also makes your body less responsive to sedation which further complicates matters. Talk to your dentist or oral surgeon if you're super nervous. Something as simple as an anxiety pill or Nitrous Oxide gas could help you calm your nerves to ease the process.
Be on Time
Dental implant surgery is a delicate process that takes a long time to perform. It's not unusual for your dentist to schedule several hours for a big implant case. Be sure to show up on time for your surgery appointment. Plan on arriving at least 15 minutes before your scheduled time. Being on time allows your dentist to take full advantage of the scheduled appointment. This way, your dentist can take his or her time to numb you properly and perform a smooth and successful surgery. Being late to your appointment puts unnecessary pressure on your dentist. This significantly increases the likelihood of running into complications down the line. Be on time, relax, and let your experienced dentist/ oral surgeon handle the rest.
No Smoking, No Vaping & No Tobacco

Smokers have way more complications with dental implant surgery as compared to non-smokers
Unfortunately for smokers, dental implants and cigarettes don't mix too well. This is because tobacco products reduce blood flow to the organs. As a result, heavy smokers have a much higher risk of implant failure, infections, and other complications following their implant surgery. We recommend that you stop smoking at least one week before and one week after your implant surgery. If you can one month, or two months, even better. This way you improve the blood flow to the organ which significantly improves the recovery process and chances of your implants taking. Talk to your dentist or physician for help on how to quit smoking.
What should you do after your implant surgery?

Be sure to follow your dentist's post-op instructions to ease the recovery process
Recovery from implant surgery takes anywhere from two to three days up to two to three weeks. Your dentist should give your some verbal and/or written instructions on what to do after the surgery. Be sure to follow your dentist's instructions carefully to minimize post-operative pain and expedite the healing process. Here are some helpful hints on what to do after your surgery:
Continue Taking Your Medications
Be sure to take your antibiotics on time until they are all gone. Just because the pain goes away does not mean that you should stop taking your antibiotics. You can however discontinue your painkillers once the pain goes away. If you discontinued your blood thinners, you could probably start taking them again two to three days after the surgery. Be sure to follow your physician's recommendation when it comes to that.
Avoid the Surgery Site
Obviously, you want to take it easy on the surgery site for the first few days. Here's a list of things you should avoid during the initial recovery period:
- Don't chew hard foods, especially things like nuts, bread, raw vegetables, etc.
- Avoid forceful spitting, rinsing, and swishing for the first few days after surgery
- Do not touch or play with the implant with your tongue or anything else
- Avoid strenuous exercise for several days
- No brushing on the surgery site for a few weeks
- Do not use an electric toothbrush or a Waterpik on the surgery site for a few weeks
It's best to avoid the surgery site as much as you can. You should probably get used to chewing mashed and soft foods for a while. Your dentist will instruct you when it's safe to resume your normal diet and oral hygiene routine.
Get as Much Rest as Possible
Just like with any other surgery, your body needs time to recover from implant surgery. Resting and relaxing are essential to a speedy recovery process. Try to get as much rest as possible during the first few days following implant surgery. Stay away from chewing hard and sticky foods to give your jaws time to relax.
Be Ready to Deal with Pain & Discomfort
Everybody responds differently to their implant surgery. Sometimes the pain lasts just two to three days after surgery. Other times it can last for several weeks. There are many different factors that impact how much pain you feel after implant surgery. Here are a few key factors that determine your pain level:
- Infection in the mouth
- Duration of surgery
- Quality of your jawbone
- Number of implants being placed inside the mouth
- Other surgical procedures that are performed in conjunction with dental implants, such as bone grafting, tooth extraction, etc. add to the pain level
- Long-term smokers almost always experience more pain
- Your medical history, such as suffering from diabetes, increases pain levels
Be sure to follow your dentist's recommendations to improve your chances of making a quick and speedy recovery.
Use Ice-Packs & Heat-Packs
Ice packs and heat packs are effective at reducing swelling and pain following implant surgery. Try icing the surgery area for the first two to three days. Place the ice pack on for 20 minutes, and off for 20 minutes. After the 3rd day, you can start applying a heat pack if still experiencing significant pain and swelling.

Place an ice pack for 20 minutes on and 20 minutes off
When should I see my dentist next?
Your dentist or oral surgeon should schedule a follow-up appointment after your surgery within one to three weeks. It's normal to experience pain, swelling, loose stitches, minor bleeding, etc. as part of the recovery process. Feel free to contact your dentist to ask questions. However, understand that there's not much they can do during the first few days of recovery. For more serious complications, such as uncontrollable bleeding, unbearable pain, or numbness at the surgery site, you should schedule an emergency visit with your dentist. If you can't get a hold of your dentist you may have to go to the emergency room instead. We hope this helps, and we wish you a speedy recovery.

0 Comments